Medical Tourism for Americans: A Financial Planner's Guide to Getting Care Abroad
Originally published April 24th, 2026; edited and republished on April 27th, 2026.
Can you really save tens of thousands of dollars getting medical care in another country? If so, when is it worth it?
With the seemingly never-ending rising cost of healthcare in the United States, medical tourism has quickly become a more viable financial strategy that many Americans had never previously considered. Today, we’ll cover who it makes sense for, which procedures travel well, how to find reputable facilities, the costs, and the risks.
What is medical tourism?
Medical tourism is just what it sounds like: it’s the practice of traveling to another country to receive medical care. For most Americans, the driver for doing this (and likely why you’re reading this post) is the potential cost savings. US healthcare prices are among the highest in the world — often five to ten times what the same procedure costs at a high-quality private hospital abroad. This isn’t news to Americans who practice medical tourism. More than three million Americans travel to Mexico alone each year for treatment. Hundreds of thousands more head to Thailand, India, Costa Rica, Colombia, and beyond.
That being said, medical tourism isn't right for everyone or every situation. Much of the written content out there on the subject provides a partial perspective, or either over- or undersells the concept. This guide is my attempt to do it right, from a practical and financial perspective. The decision ultimately rests with you, your loved ones who might support you on your healthcare journey, and your healthcare providers.
➡️A note before we start: Neither I nor anyone in my firm is a physician, and nothing here is medical advice. Serious considerations of medical care abroad should begin with a conversation with your doctor.
Who medical tourism actually makes sense for
Medical tourism is primarily a financial decision — and whether that decision makes sense depends almost entirely on your financial situation and your insurance coverage. While these can vary widely, let’s break it down into three main financial profiles. See which one fits you the best.
Profile 1: Low income, low assets — probably not the right move
This might seem counterintuitive, but the US hospital system actually has safety nets for people with low income and/or low assets. Roughly 80% of US hospitals offer charity care programs. These are free or heavily discounted care for patients who can't afford to pay. Eligibility for charity care is typically based on income below 200–300% of the federal poverty level, which is roughly $30,000–$45,000 for a single individual. And some hospitals are even more generous than that.
This isn’t hypothetical, either: I made use of hospital charity care when I was young, single, and living paycheck. Like too many Americans, I was caught off guard by an unexpected health emergency. Charity care didn’t cover every expense associated with my hospital stay. I still had to find a way to pay for various lab tests, exams, the emergency room, and the ambulance ride. But it took care of the biggest things.
Beyond charity care, the practical reality of medical debt collection means lower-income patients with few assets often face limited consequences even when their bills go unpaid. Hospitals know that more than half of all hospital bills never get paid in full. Someone with no significant assets, lower income, and possibly little to no home equity is probably not in a situation where they have to worry about collections too heavily.
For a person in this scenario, traveling abroad for a complex medical procedure — possibly alone, while sick, and navigating a foreign healthcare system — may not only add risk and logistical burden, but could end up costing more or being a wash compared to staying home and receiving care. If this sounds like you, medical tourism is probably worth passing on for most of your essential healthcare.
Profile 2: Middle income, moderate assets — the group with the most to gain (and lose)
This is where medical tourism has its most compelling financial case. But, it’s also where the stakes of getting it wrong begin to rise.
The person in this profile likely earns too much to qualify for charity care at a US hospital — maybe $60,000 to $150,000 household income. If this sounds like you, you have a home, some retirement savings, and a modest emergency fund. You’re financially stable, at least in normal times. But you don't have the cushion to absorb a $150,000 to $500,000 medical bill, which is what uninsured cancer treatment or a major surgery can realistically cost in the US.
These are people who did everything right. They built some savings. They own a home. They have something to lose, because they have enough assets to be worth pursuing in a collection action, enough income to be ineligible for most assistance programs, but not enough financial liquidity to absorb a catastrophic medical bill without life-altering financial damage.
A person that fits this profile is likely uninsured or underinsured due to being self-employed, in between jobs, or associated with a small employer that doesn’t offer health insurance as a benefit.
For this group, the savings available through medical tourism — often 50–80% on major procedures — can be the difference between financial survival and financial devastation, even when you add in travel costs. Saving money on expensive treatment can be the difference between retiring in a few years or in fifteen. It can be the difference between supporting a child through college.
➡️ What about paying other bills? To be sure, medical tourism can save you loads of money on treatment. If you have disability insurance, the logic of seeking treatment becomes even more clear. Disability benefits replace a portion of your income while you're unable to work (subject to certain conditions such as waiting periods, and limits such as coverage duration.) This means during a cancer treatment period abroad, your living expenses may be partially covered — even fully covered, if you’ll be traveling to a lower cost of living area of the world. Not only are you saving money on treatment, you're not simultaneously losing income. If you have a disability insurance in place, but lack the health insurance to self-insure a six-figure medical bill, you could be the ideal medical tourism candidate.
Profile 3: Higher net worth / self-insured by choice: your call
At certain levels of wealth and income, it's less of a survival decision and more of a preference and values decision. Someone with substantial liquid assets (generally very comfortable amounts of money in cash and bank accounts) might just find it easier to choose to pay for US treatment for the purposes of care continuity, and proximity to family and social support — even without insurance. Or they might go abroad because saving $80,000 is still $80,000. There’s no right answer here, but the financial driver isn’t as much for someone with moderate means.
➡️ Hypothetical example: dental work.
You need around $12,000 of dental work. Your insurance maxes out at $1,500 per year.
A crown ($1,800), a root canal ($1,800), and two implants ($4,000–$6,000 each) add up fast. Your insurance covers maybe $1,500 of it. You've been putting this off for two years. This is a potentially strong financial case for medical tourism. Traveling to Costa Rica or Mexico isn’t far, and the cost savings can be substantial.
A quick note on medical debt
One thing worth understanding: medical debt being uncollected doesn’t mean it’s consequence-free. In most states, hospitals and medical debt buyers (yes, these exist, sadly) can and do sue patients to collect on unpaid bills. A middle-income person with a home, retirement accounts, and a paycheck is exposed to risk in ways a low-income person with no assets isn't. (Whether retirement accounts are exposed to collection varies by state.)
Various safety nets generally catch people with lower means. The people most financially exposed to a catastrophic medical bill are the ones those safety nets won’t catch, and whose personal safety nets won’t catch them either. These are the ones medical tourism is for.
Step one: figure out what it would actually cost you at home
Before you can compare medical tourism against staying in the US, you need an idea of what your out-of-pocket costs in the US will actually be. Fortunately, you can just walk into a hospital and look at the menu. (I’m totally kidding, I wish it were that easy.)
I once called my local hospital system and asked for a full list of costs, which they provided with the caveat "but no one actually pays that." The numbers they gave me are chargemaster prices — basically, the hospital's list price, inflated largely to give insurers room to negotiate it down. It bears almost no relationship to what an insured patient pays (which is maddening in and of itself.) For uninsured patients who get billed at the full rate, those costs can look scary — even a self-pay discount might not put much of a dent in them.
Here’s how to go about getting some real numbers.
If you have insurance: Your insurer's member portal almost certainly has a cost estimator tool. This is the most accurate option available to you because it uses your specific plan's negotiated rates and your current deductible status. Log in, find the cost estimator, search for your procedure, and filter for in-network providers. The number it gives you reflects what you'd actually owe. You can also call member services (typically printed on your health insurance card) for assistance finding and using the tool, or sometimes, getting a cost estimate directly.
For a general benchmark: FAIR Health Consumer at fairhealthconsumer.org is an independent nonprofit tool that lets you search procedure costs by zip code. It shows both insured and uninsured cost estimates based on actual claims data in your area. It won't match your specific plan exactly, but it gives you a legitimate ballpark. No login or fees to use this service, which is nice.
If you're uninsured: You're entitled under the No Surprises Act to request a good faith cost estimate from any provider before a scheduled procedure. Ask for it in writing. The number they give you is supposed to reflect your actual out-of-pocket cost, not the chargemaster price. It's also a starting point for negotiation — many hospitals will discount cash-pay rates significantly if you ask directly, because a discounted cash payment today is worth more to them than a collection action later.
The honest caveat: Even with all these tools, your US estimate will always be fuzzier than an abroad quote. International patient departments at foreign hospitals compete on price clarity and typically give you an all-inclusive number upfront. Your US number depends on your plan, your deductible status, and whether every provider involved — surgeon, anesthesiologist, facility — is actually in-network. The anesthesiologist out-of-network surprise bill is a real and common problem. You can be in-network at an in-network hospital and still receive an out-of-network bill from someone who walked into your operating room.
Get the best US estimate you can, then compare it honestly to the all-in abroad number including travel. That's the only comparison that tells you anything useful.
Not all medical care is right for travel
Medical tourism works best for planned, elective procedures with a defined treatment timeline. It works second-best for necessary, but non-urgent procedures. It works least well — and in some cases not at all — for urgent or emergency situations.
The obviously impractical
Anything time-sensitive or emergency-related makes no sense for medical tourism. Heart attacks, strokes, acute trauma from an accident or injury, and any situation where your condition could deteriorate rapidly — either during the travel planning process, or during a long-haul flight — are not really candidates. Mid-stream treatment is also risky. If you're already three months into a chemotherapy protocol with a US oncologist, disrupting that relationship carries real risk, and you’ll likely be advised against it.
Procedures that ‘travel well’
Dental work is the single highest-volume medical tourism category, and often the most financially compelling. A single dental implant costs $3,500–$6,000 in the US; the same implant costs $700–$1,500 in Mexico or Costa Rica. Full-mouth reconstruction or All-on-4 implants that run $40,000–$60,000 in the US can be done for $10,000–$20,000 abroad including travel.
Orthopedic surgery — hip and knee replacements are among the most common procedures Americans seek abroad. A hip replacement averaging $28,000–$60,000 in the US costs $5,000–$11,000 in India, Mexico, or Thailand.
Cosmetic and plastic surgery — breast augmentation or reduction, rhinoplasty, facelifts, tummy tucks. These savings are especially significant because US insurance doesn't cover elective cosmetic procedures at all. A facelift costing $25,000 in Beverly Hills runs $4,000–$6,500 in Colombia. A little beyond the scope of this post, but still important to know since there can be substantial cost-savings if these procedures feel important to your well-being.
LASIK eye surgery — quick, well-standardized, and dramatically cheaper abroad. LASIK for both eyes runs $4,000–$5,000 in the US. In Turkey: $800–$1,200. Mexico: $1,500–$2,000.
Bariatric surgery — gastric sleeve averages $15,000–$25,000 in the US. In Mexico, all-inclusive packages from board-certified surgeons at accredited hospitals start around $3,900–$6,000.
Fertility treatments (IVF) — this one surprised me in this research process, because it was one I hadn’t even considered. A single IVF cycle averages $15,000–$20,000 in the US, often not covered by insurance. Also, couples generally need more than one round. The Czech Republic and Spain offer complete cycles for $3,000–$7,600, with English-speaking staff and European-standard facilities. Of course, the catch is that your embryos will be stored overseas. But on the plus side, overseas embryo storage is also cheaper than in the US.
Orthodontics / Invisalign — Invisalign runs $5,000–$8,000 in the US. Abroad, the same Align Technology product costs $1,800–$5,000 depending on case complexity and destination. The logistics require at minimum two trips (initial fitting and one follow-up for refinements), with virtual check-ins in between.
For children's braces: Traditional wire braces require in-person tightening every 4–8 weeks and are generally not practical to manage entirely abroad, unless your family already plans to live abroad for other reasons. Here’s one US Orthodontis’s cautions on starting abroad then transferring care to the US.
Cancer: complicated, but worth considering in specific scenarios
Because of the variety of cancer types and corresponding treatment options, this deserves its own section.
For a lot of cancers, there is time to plan. The national average from diagnosis to beginning treatment at US academic medical centers is already close to six weeks. A well-organized patient pursuing medical tourism may not actually be any slower than someone navigating the US system's own bureaucracy.
That said, some cancers require urgent action and aren’t appropriate for medical tourism.
Do not delay: Some cancers require treatment to begin within days of diagnosis. Others are slow-moving enough that weeks of planning time are reasonable. Your oncologist is the right person to tell you which situation you're in. Have this conversation before beginning travel plans.
If reasonable planning time exists: For other diagnoses, planning time exists. How much depends on your specific type, stage, and other factors. Your oncologist will be able to tell you what your window actually looks like.
The financial case for cancer treatment abroad is strongest for the middle-income uninsured patient, and for someone who also has disability insurance to replace income during treatment. A person staring down a $300,000 cancer treatment bill with no insurance, some retirement savings, and a home is in real financial jeopardy. The same treatment in India, Germany, or Israel at 70–80% less may preserve their financial life and their physical one.
➡️ Hypothetical example: hip replacement with a high-deductible health plan.
You're 52, self-employed with a high-deductible health plan, and your doctor says you need a hip replacement.
Your HDHP out-of-pocket maximum is $7,500 — if the total bill stays in-network and your insurer agrees on what's covered. The actual out-of-pocket could be much higher. Without insurance: $28,000–$60,000. In India or Turkey, all-in: $5,000–$10,000. Even accounting for flights, hotels, and meals, that can be big savings.
➡️ Hypothetical example: IVF not covered by insurance.
You're 34, have been told IVF is your best option, and your insurance doesn't cover it.
One round in the US: $15,000–$20,000, and most couples need more than one. The Czech Republic: $3,000–$4,900 per cycle. Spain: $4,300–$7,600. For couples who need three rounds, that's potentially $30,000–$45,000 saved, and that’s with with European-standard facilities, English-speaking staff, with no visa required for US citizens (the Czech Republic and Spain are both areas that allow Americans to enter visa-free for up to 90 days with just a passport.)
Lesser-known procedures worth considering
Beyond the headline categories, there's a longer list of procedures Americans routinely put off, pay too much for, or go without entirely that travel surprisingly well.
Sleep apnea surgery is one that deserves more attention than it gets. Most people with obstructive sleep apnea have lived with it for years before seriously considering surgery. (Like me! No more CPAP!) That means there's less urgency and more planning time. The most common surgical procedure for sleep apnea costs $10,000–$15,000 in the US. The new and increasingly popular Inspire implant can exceed $40,000–$50,000 including surgery. Both are available at significantly lower cost at accredited facilities in Thailand, India, and Costa Rica. And recovering for two weeks in a warm climate after a procedure you've been putting off for a decade isn’t a bad bonus.
Cochlear implants and hearing loss treatment. Cochlear implant surgery in the US commonly runs $50,000–$100,000+. In India, the same surgery at a JCI-accredited facility costs $15,000–$25,000, often with the device included. For someone who has been delaying this because of cost, that’s a lot of savings. And once again…some time away from home doesn’t hurt either if you like to travel.
Arthroscopic surgery for things like knees, shoulders, or hips. This type of procedure is less involved than a full joint replacement, but the same cost logic applies. Arthroscopic knee surgery for meniscus repair or ACL reconstruction runs $10,000–$30,000 in the US. In Thailand or Mexico at an accredited facility, the same procedure runs $3,000–$8,000.
Varicose vein treatment. Often not covered by US insurance unless the condition is severe enough to meet clinical criteria. The procedures runs $1,500–$3,000 per leg in the US. Abroad, the same procedures cost a fraction of that and are quick outpatient procedures with easy recovery.
Fertility treatments beyond IVF. Egg freezing, embryo storage, ICSI, and egg donation all follow the same cost logic as IVF. Spain in particular has built a sophisticated fertility ecosystem serving international patients, with the largest available donor pool and transparent package pricing.
Gender-affirming surgery. Long wait times, frequent insurance denials, and very high US costs have made this one of the fastest-growing medical tourism categories. Thailand has world-renowned surgeons for these procedures, many of whom have trained specifically in this specialty and have higher procedure volumes than most US surgeons.
Addiction treatment and residential rehab. Another one that surprised me. High-quality residential treatment programs in Thailand and Mexico cost $3,000–$8,000 per month. The same caliber of program in the US runs $20,000–$60,000 per month. For someone who needs 30–90 days of residential treatment, the difference is enormous.
Stem cell therapy: proceed with caution. Some experimental stem cell therapies in the US are also offered at clinics abroad. But be warned: patients with conditions like multiple-sclerosis, ALS, or Parkinson's are the target market for predatory operators who count on peoples’ desperation. Be cautious of testimonials over clinical data - it’s a big red flag. Bottom line is that stem cell therapy abroad is just riskier, and requires more due diligence.
If you're seriously considering this, three concrete steps: check out clinicaltrials.gov to see if the treatment appears as a registered trial. Read the international society for stem cell research (ISSCR)'s patient guide at isscr.org/patients. It's written for a general audience, it’s credible, and it’s independent. Lastly, understand what you may be giving up: receiving unregulated stem cell treatments abroad may disqualify you from enrolling in future approved clinical trials for the same condition. Sounds crazy, but it’s a real risk.
➡️ Hypothetical example: sleep apnea surgery.
You've had sleep apnea for years. Your doctor recommends surgery.
You've done the CPAP. It's not working for you. Surgery in the US: $10,000–$15,000. The Inspire implant: $40,000–$50,000. These procedures are available at accredited facilities in Thailand and Costa Rica at 50–70% less. If you’re not in a hurry, and have time to research/plan/book a trip, getting it taken care of abroad could be worth considering. Recovering on the beach is a nice bonus.
What if you’re on Medicare?
Medicare generally does not cover healthcare services received outside the US or its territories, with three narrow exceptions involving emergencies near the Canadian or Mexican border and care on cruise ships within six hours of a US port. For planned procedures, Medicare beneficiaries are paying entirely out of pocket — the same as the uninsured.
But Medicare has its own significant coverage gaps, and those gaps are exactly where medical tourism makes sense for older Americans.
Dental procedures: Original Medicare excludes most dental procedures including cleanings, fillings, and dentures. Medicare Advantage plans vary, but even among those that include dental benefits, nearly half have annual maximums of $1,000–$1,500 — irrelevant for major dental work. When a single implant costs $4,000–$6,000 and full-mouth reconstruction can run $40,000–$60,000, those caps barely make a dent in the overall cost.
This makes dental tourism one of the most compelling medical tourism categories for Medicare-age Americans. The procedure they most need, Medicare won't cover, and the savings abroad are enormous. A full-mouth reconstruction in Costa Rica or Mexico at $10,000–$20,000 versus $40,000–$60,000+ at home — with zero insurance involvement on either end — is a pure out-of-pocket comparison, and it isn't close.
Orthopedics with high cost-sharing: Medicare does cover hip and knee replacements, but beneficiaries without a strong Medigap supplement can still face $3,000–$7,000+ in out-of-pocket exposure. But for something like this, there may not be big cost-savings for completing procedures abroad. It all depends on what’s covered under an Advantage plan or supplement.
➡️ Hypothetical example: uninsured and in need of a hip replacement.
You're 52, no health insurance, and the doctor says you need a hip replacement.
Without insurance in the US: $31,000–$45,000, billed at full rates with no negotiated discount and no cap on what you owe. In India or Thailand, all-inclusive at an accredited facility including flights and hotel: $8,000–$13,000. Net savings: $20,000–$35,000. The case here is about as clear as medical tourism gets.
But be warned: the math changes if you have insurance. With a high-deductible plan, your out-of-pocket might be $3,000–$9,000 depending on where you are in your plan year. That means going abroad could actually cost you more once travel is factored in. Run your specific numbers before assuming the abroad option wins.
Cataract surgery: If you need cataract surgery and Medicare covers it, you'll get a standard lens that fixes the cloudiness. What Medicare won't cover is the upgrade to a premium lens, which is the kind that also corrects astigmatism or reduces your dependence on reading glasses afterward. That upgrade runs $1,000–$4,000 per eye out of pocket, and Medigap won't cover it either.
Getting it done abroad can mean cost savings, but they aren’t as dramatic as some other procedures we’ve discussed. Premium lens cataract surgery in Mexico runs $1,000–$2,200 per eye all-in. Thailand is similar. For someone paying $2,000–$3,000 per eye at home for the upgrade, the savings net of a short trip aren’t enormous, but they’re there. Where it gets more interesting is if you need surgery on both eyes, and you're facing the full upgrade cost twice. At that point a trip to Mexico starts looking reasonable, especially if you'd been planning to go anyway for other dental work, vision work, or just to get away.
One thing Medigap policyholders should know: some Medigap plans include a foreign travel emergency benefit with a $250 annual deductible, after which the plan covers 80% of eligible emergency care costs abroad. This is specifically for emergencies, not planned procedures. But it does mean a Medicare beneficiary with good Medigap coverage has at least some protection if something goes unexpectedly wrong while abroad for elective care.
➡️ Hypothetical example: on Medicare and need lots of dental work.
You're 68, on Medicare, and need full-mouth dental reconstruction. Your Medicare Advantage plan covers $1,500 per year in dental benefits.
Your $1,500 annual maximum won't touch a full-mouth reconstruction that costs $40,000–$60,000 in the US. In Costa Rica or Mexico, the same work costs $10,000–$20,000 all-in including travel.
Talk to your US doctor first
Before you research facilities, price procedures, or book flights, talk to your primary care physician.
Tourists sometimes don’t inform their doctor before going abroad for a procedure, because they’re afraid of being told not to proceed, or they simply don’t think about it. But it’s an important thing to do, for your sake. The American Medical Association's own ethical guidelines specifically instruct physicians to advise patients who inform them in advance whether they are willing to provide follow-up care. This means if you don't tell them, you may return home to find your own doctor unprepared or unwilling to continue your care.
Your doctor can help you assess whether the timing of your procedure is medically safe for travel, what records you'll need to bring, what to look for in a foreign provider, and what follow-up care will be needed when you return. They might have reservations, depending on their familiarity with medical tourism, but they might also have important input from experience. Think of it less as asking permission and more as doing pre-trip reconnaissance.
A quick reference for matching your procedure to the destinations where it's most commonly and cost-effectively performed. Savings ranges are approximate versus US self-pay rates. Sources: Medical Tourism Magazine, Patients Beyond Borders, Grand View Research, ScienceInsights, PharmiWeb, centralamerica.com.
| Destination | Best known for | Typical savings vs. US | Practical note |
|---|---|---|---|
| Latin America | |||
| MexicoTijuana · Los Algodones · Monterrey | 60–80% | Closest option for most Americans. Strong English-speaking infrastructure in border cities. Best value for bariatric surgery in Latin America. | |
| Costa RicaSan José | 40–70% | Established dental tourism infrastructure, English widely spoken, short flight from East Coast and Southeast. | |
| ColombiaBogotá · Medellín | 50–80% | Highest concentration of JCI-accredited hospitals in Latin America. Fundación Santa Fe de Bogotá ranked #1 for orthopedics in the region by Newsweek/Statista 2025. | |
| Europe | |||
| TurkeyIstanbul · Ankara | 60–75% | Dominant global destination for hair restoration — 2M+ medical tourists in 2024 per Turkish Health Ministry. Quality varies significantly; JCI accreditation matters more here than almost anywhere else. | |
| HungaryBudapest | 40–60% | The "dental capital of Europe." Decades of established infrastructure serving Western European patients. Market projected to grow 15% CAGR through 2030. | |
| Czech RepublicPrague | 40–60% | Popular for lower-cost donor-egg IVF. High medical standards, EU-regulated environment, Prague is easy to reach from major US hubs. | |
| SpainMadrid · Barcelona | 30–55% | Major IVF hub — permissive legal framework and abundant anonymous egg donors make Spain the top European destination for donor-egg IVF. Strong oncology and orthopedic programs. | |
| GermanyFrankfurt · Munich · Berlin | 0–30% | Premium tier — chosen for access to treatments and diagnostics not widely available in the US, not primarily for cost savings. University hospital system is among the strongest in the world. | |
| Middle East | |||
| IsraelTel Aviv · Jerusalem | 0–25% | World leader in oncology and fertility; Sheba Medical Center ranked among top global hospitals. Chosen for quality and access to cutting-edge protocols, not cost. Israel leads the world in IVF cycles per capita. | |
| Asia | |||
| IndiaChennai · Mumbai · Delhi · Bangalore | 70–90% | Most dramatic cost differential of any destination — cardiac bypass $7K–$15K vs. $120K in the US. Apollo and Fortis hospital networks are JCI-accredited and serve 200,000+ international patients annually. English widely spoken. | |
| ThailandBangkok · Phuket | 50–70% | One of the longest-established medical tourism destinations. Bumrungrad International (Bangkok) pioneered international patient infrastructure. Broad procedure menu with strong JCI presence. | |
| MalaysiaKuala Lumpur · Penang | 50–70% | Strong JCI presence, English widely spoken, competitive pricing across a broad range of procedures. KPJ Healthcare and Sunway Medical Centre well-regarded for international patients. | |
| South KoreaSeoul | 30–60% | Global leader in facial cosmetic surgery and precision aesthetics — techniques and procedures not widely available in the US. Samsung Medical Center among top-ranked globally for oncology. | |
| SingaporeSingapore | 10–30% | Premium tier alongside Germany and Israel. Government-supported medical tourism infrastructure; Mount Elizabeth and Gleneagles are internationally recognized. Chosen for quality and access to advanced care, not primarily cost. | |
Savings percentages are approximate versus US self-pay (uninsured) rates and will vary by procedure, facility, and individual circumstances. Insured patients may see smaller or no savings depending on their coverage. Always verify current JCI accreditation status at jointcommissioninternational.org before selecting a facility.
How to find a reputable facility
The most important credential to look for is JCI accreditation — Joint Commission International, the same body that accredits US hospitals, applied internationally. JCI evaluates hospitals on patient assessment, care delivery, surgical procedures, medication safety, infection control, and staff qualifications. A JCI-accredited hospital abroad is operating under standards genuinely comparable to a US hospital.
How to verify: The Joint Commission International maintains a complete, searchable public database of every currently accredited organization on the website. The list is searchable by country, city, and organization type. The key word here is currently. It’s important to know that accreditation requires ongoing compliance. Don’t trust that an organization is JCI accredited just because their website says so. Always verify directly on JCI's site rather than relying on a facility’s marketing material or word.
JCI accreditation isn’t a niche thing, either. More than 1,000 healthcare organizations in over 70 countries hold current JCI accreditation. There are other organizations that provide international accreditation, but JCI is the one your doctors are most likely to recognize.
Beyond accreditation, you can do further vetting by asking about your specific surgeon:
How many of your types of procedure do they perform each year?
How long have they been practicing?
Research shows that higher-volume surgeons have better outcomes, fewer complications, and lower revision rates. What counts as "high volume" varies, depending on what you're having done. The right number for a hip replacement is different from the right number for heart surgery, for example.
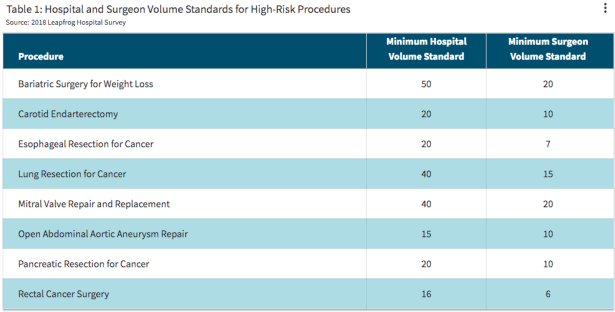
One potential starting point is the Leapfrog Group (leapfroggroup.org), a nonprofit patient safety organization that publishes procedure-specific volume standards for common surgeries — written specifically for patients and employers evaluating providers. It won't cover every procedure, and it’s done on American hospitals. But gives you a benchmark to ask against for certain high risk procedures. You can also ask your doctor how you can find volume benchmarks for your specific procedure.
The bottom line is that there are just limits when you ask a foreign hospital's coordinator how many procedures their surgeon performs annually. You're relying on their answer. Unfortunately, there's no independent international registry you can verify it against. That's why the best use of whatever information you collect is to bring it back to your US physician and ask their read on it. Let them review what you’ve gathered, and ask them if it feels reasonable. But JCI accreditation is probably the safest fallback.
Should you use a medical tourism facilitator or travel agent?
A medical tourism facilitator is a company that acts as a coordinator between you and foreign healthcare providers. This is a company that can handle hospital selection, appointment logistics, records transfer, local transportation, accommodation, and sometimes eveninsurance. Think of them as somewhere between a travel agent and a patient advocate, with varying degrees of both.
They're a legitimate and growing industry, and for the right situation they can take some decision-making off your plate (after all, you’re already thinking about a medical procedure.) But beware: they can also add cost and a hidden conflict of interest.
Commissions: Medical tourism facilitators earn money one of two ways. Some charge you a direct fee — typically $1,500–$5,000 — for their coordination services. Generally, this is the better way to go because it’s just more transparent. But they earn a commission from the hospitals and clinics they refer patients to, built into the price you're quoted. The facility charges the facilitator a higher rate than their standard price to absorb that commission — often $5,000–$10,000 more than you'd pay booking directly — and the facilitator presents it to you as the going rate. The risk here is that you don’t even know it’s a markup. And why would you? You have nothing to compare it to.
This is why the Medical Tourism Association (yes, that exists too) recommends clear, transparent contracts. You can read more about their thoughts here.
🚩 What to ask if you use one: Having a straightforward dialogue with one of these companies before hiring them is sometimes just the best place to start. Ask them:
Do you earn a commission from the facilities you recommend, and how much?
Do you have relationships with multiple providers for my procedure, or just one?
Are the hospitals you recommend JCI-accredited?
If they’re reluctant to answer any of these, that’s a red flag, and you should pass on their services.
When they're worth it: For common procedures, you probably don't need a facilitator. The hospitals have dedicated international patient departments built for exactly this, JCI verification is a quick five-minute search, and the logistics of a short trip to a nearby country are manageable independently. Where a facilitator earns their fee is when the situation is more complex than usual. For example: cancer treatment requiring extended coordination, multi-procedure trips, destinations where there’s a language barrier, or if you’re just not comfortable navigating travel without some help.
An additional resource: Patients Beyond Borders (patientsbeyondborders.com) operates as an independent guide and educational resource. Its founder has been writing about medical tourism for nearly two decades and the site covers destinations, procedures, and facility vetting with less commercial conflict than some facilitators. It's a starting point for further research, regardless of whether you end up using a facilitator. They even have a full list of vetted clinics you can review on their website.
Passports and visas: what to know
Passports
If you don't have a current passport, it’s wise to get one now instead of waiting until you need it. A passport is $130–$165, valid for ten years, and represents one of the most high-value, low-cost insurance policies available to you. Routine processing currently takes 4–6 weeks. Expedited processing costs an extra $60 and takes 2–3 weeks, not including mailing time in either direction.
Most Americans can obtain a passport without issue. The narrow exceptions: people with outstanding felony warrants, those on parole or probation with travel restrictions, and those who owe $2,500 or more in child support.
Visas: good news for most people
For the most popular medical tourism destinations, Americans face little to no visa bureaucracy:
Mexico: No visa required. Americans can stay up to 180 days. That’s long enough for the vast majority of procedures, including built-in recovery time.
Thailand: Visa-free for up to 60 days. Thailand also offers a dedicated Medical Tourist Visa for $40–$80 allowing 60–90 day stays with straightforward paperwork.
Costa Rica: Visa-free for up to 90 days.
Colombia, Turkey, Germany, Spain, Portugal, Czech Republic: All accessible without a tourist visa or with simple e-visa processes.
India: Offers a dedicated Medical Visa (M-Visa) for patients and companions, designed for longer treatment stays.
The bottom line here is that getting your passport or renewing is the easiest and most cost-effective first step. The most popular medical tourism destinations tend to very traveler-friendly when it comes to visas.
Select your nearest airport and a destination from the dropdowns, or click any dot on the map.
Select an airport and destination to see flight details.
Flight times are approximate averages. Actual times vary by airline and routing. Layover likelihood reflects typical booking patterns — direct service may be available on select carriers or dates.
Determining the true cost
The cost savings in medical tourism are real, but the headline numbers like"80% less!" don't tell the full story.
Expect total travel-related costs to run 30–50% on top of the procedure cost itself. That includes flights, accommodation for the duration of your stay, meals, local transportation, medical tourism insurance, prescription costs, post-operative care at the foreign facility, and the cost of bringing a companion if you decide to.
Don’t worry: the math still works well for high-cost procedures. A $123,000 heart bypass in the US versus $7,000 in India, even with $5,000 in travel overhead, is a $111,000 difference. A $40,000 hip replacement versus $8,000 in Thailand plus $3,000 in travel costs is still a $29,000 difference. For lower-cost procedures, the savings get thinner relative to the trouble involved, so you’ll have to weigh the pros and cons a bit more carefully.
➡️Hypothetical example: weight loss surgery not covered by insurance.
Your doctor recommends weight loss surgery. Your insurance won't cover it until your BMI hits a higher threshold.
US gastric sleeve: $15,000–$25,000 out of pocket. Mexico, all-inclusive with a board-certified surgeon, accredited hospital, and a short drive of the US-Mexico border: $3,900–$6,000.
Medical tourism insurance: what you actually need
Medical tourism insurance is essential because standard travel insurance does not cover planned medical procedures abroad. The most well-known companies for travel insurance like Allianz, GeoBlue, IMG exclude routine, preventative, or elective care. Only unforeseen emergency medical costs are covered.
The same is true of your US health insurance. HMO plans have zero foreign coverage. Medicare has zero foreign coverage. Many ACA marketplace plans exclude foreign care entirely.
What you need for planned medical procedures is a specific product called medical tourism insurance, which is designed specifically for patients traveling abroad for planned procedures.
What your medical tourism insurance should cover
Complications from your planned procedure, both while abroad and after you return home. Medical complication benefits typically extend 180 days after the elective procedure, with additional coverage for complications up to 270 days from the original surgery date.
Medical evacuation, like an air ambulance transport if the local facility can't handle a complication. Air ambulance from a foreign country to the US can cost $100,000–$250,000. Your policy should cover at least $250,000 in evacuation benefits.
Trip cancellation or interruption: if the hospital cancels your surgery date or you develop a condition that prevents travel.
Extended stay coverage: if your recovery takes longer than planned due to a complication.
What it costs and when you need it
Premiums can vary, like with all insurance. But a medical tourism policy might run $500–$1,500. It will depend on the procedure, coverage limits, and duration. It’s an extra expense, to be sure. But it’s worth it considering the hundreds of thousands of dollar unplanned expenses it can be protect against.
You’ll want to review the policy you’re considering and compare it to the procedure you’re having. Have a conversation with you doctor about the possible risks to determine what type of coverage, if any, is appropriate. In some cases, it’s a no-brainer. For lower-risk procedures, you may decide to forgo it.
One important timing note: You must purchase medical tourism insurance before you leave your home country. Some providers allow mid-trip purchases but apply a 48-hour waiting period. This is to prevent people from buying insurance only after a complication has already occurred.
Where to find it
This is a niche product and it is not on the shelf at your local insurance agent.
Global Protective Solutions (GPS): an established dedicated medical tourism insurance providers, covering travel accident and medical complications for patients undergoing elective procedures outside their home country. Available at globalprotectivesolutions.com.
Sylk Health: a newer platform specifically focused on medical tourism patients with transparent coverage comparisons at sylkhealth.com.
Your medical tourism facilitator: some established facilitators have relationships with insurers and include coverage in packages. If you’re using a facilitator, ask them what they recommend. But review the policy yourself.
💬When comparing policies, ask:
Does it explicitly cover complications from a planned elective procedure?
What are the coverage limits — is $100,000 enough for your procedure?
Does post-return complication coverage extend to treatment back in the US?
What is the claims process if something goes wrong abroad?
Privacy and your medical records
HIPAA doesn't travel with you
HIPAA is a US law. It protects your health information in US facilities. When you receive treatment abroad, your records are governed by that country's laws — which range from robust (the EU's GDPR is arguably stricter than HIPAA in certain respects) to minimal in some popular destinations.
It’s less about data breaches, and more about how the foreign facilities handle your information. In some cases, the risk will just be higher. That may be a tradeoff you’re forced to make.
What to bring home after your treatment
Unlike the US healthcare system, which has records-sharing systems such as Epic, you are the liaison between your foreign care and your US care. Epic is working to expand abroad, but for now, you should plan to carry your records with you.
Before leaving the foreign facility, get:
Complete operative or treatment notes in English. Ask for a translation, or prepared to do some translating yourself with an AI tool or professional translator. Since AI can make mistakes, not knowing the lingo could work to your detriment. This is where a professional translation service might be worth using, if the foreign facility doesn’t offer it.
All imaging: scans, X-rays, pathology reports in digital format.
A complete medication list: every drug received, including doses, and dates.
Post-discharge instructions in English.
Implant or device documentation if applicable (manufacturer, model, serial number.)
Direct contact information for your surgeon and every specialist involved.
Contact for the facility's international patient coordinator.
Your US physician needs this information to provide safe follow-up care. Without it, even a perfectly successful procedure abroad can lead to suboptimal outcomes because your American doctor is guessing about what was done and how.
The pre-departure and post-return checklists
What do US doctors think of medical tourism?
Like all professionals, doctors are not homogenous in their opinions. But generally, the main frustration of US physicians is the challenge of follow-up care. Returning medical tourists often don't have records of the procedures they underwent or medications they received, and their US physician is then expected to manage follow-up care without the information needed to do it safely. That’s why the American College of Surgeons issued a specific recommendation: obtain a complete set of medical records before returning home.
The only way to know what your doctor will think is to ask them. Remember, their opinion is only an opinion. At the end of the day, it’s your money and your decision, and only you can advocate for yourself.
Legal recourse for medical malpractice abroad
“If your primary concern in going to a doctor, surgeon, or dentist is whether or not you're going to have legal recourse if you don't like the work you get, you shouldn't go overseas.” - Jeff Schult, Beauty From Afar: A Medical Tourist's Guide to Affordable and Quality Cosmetic Care Outside the U.S.
In most countries where Americans seek treatment, medical malpractice law isn’t as developed of an area of practice as it is in the United States. Some hospitals require patients to waive their right to sue as a condition of treatment. If you want to pursue legal action in the country where care was received, you're navigating a foreign legal system in a foreign language under laws that may barely recognize the concept of malpractice.
Suing the foreign provider in a US court is generally not viable. You'd need to establish that the foreign doctor had sufficient connections to the US for a US court to have jurisdiction, which legal experts say is a challenge.
This is a reason to choose your facility carefully, based on credentials and outcomes data rather than price alone. The legal system is a backstop you will likely not have access to. Reputation, accreditation, and your own research are going to be your main protections.
Are there horror stories?
Sort of, but these cases are almost always a cosmetic procedure done at a non-accredited facility. It is frequently at a budget clinic in a border town or tourist area. The patient chose the provider based on price, a quick Google search, or maybe even social media recommendations.
But here’s the thing: none of the documented horror stories involve JCI-accredited hospitals at established medical tourism destinations. This is why selecting a reputable, vetted facility is the best route to go.
The psychological and emotional components of medical tourism
The financial and logistical planning for medical tourism is something heavily talked about. The human reality, less so.
Research shows that social support during serious illness, especially cancer treatment, has measurable effects on both quality of life and treatment outcomes. A lack of support from family or friends can increase mortality risk after a serious diagnosis. A Facetime or Zoom call could feel like enough for some patients. But others just want someone to hold their hand at 3am when they feel nauseous.
If you're considering medical tourism for a procedure that requires an extended stay, be honest with yourself about the emotional logistics. The best facilities abroad have dedicated psychological support services, international patient lounges, and patient coordinator programs specifically designed to support international patients. But those are amenities that help on your better days. On the hard days, there is no substitute for the person you most want nearby.
The cycle structure of some treatments creates some flexibility, such as when there are rest periods between cycles. This could allow short trips home or visits from family. Planning that out in advance, before you're in the middle of treatment and trying to make decisions while sick, is important.
➡️ Hypothetical example: early-stage breast cancer with no insurance.
You were just diagnosed with early-stage breast cancer. You're self-employed with no health insurance. You have a home and retirement savings.
US treatment cost: $150,000–$300,000. You have enough assets to be worth pursuing in a collection action, enough income to be ineligible for charity care, and not enough cushion to absorb the full bill without lasting financial damage. You also have disability insurance. This is the financial profile medical tourism exists for. Israel, Germany, and India all have world-class oncology centers at 65–80% less than US prices.
➡️Hypothetical example: cancer diagnosis with employer-sponsored health insurance.
You have good employer health insurance and just got a serious diagnosis.
Your insurance will cover most of the treatment cost, your out-of-pocket max is $4,000–$6,000, and you have an oncology team already in place. Staying home might be the better choice.
Having a will and powers of attorney in place before you go
A sustained trip out of the country means it’s possible you’ll have financial needs that can’t wait to be addressed before you come home. Speak to attorney about having a financial power of attorney in place so that a trusted person can access your bank accounts and pay unexpected bills while you’re away. Many travel agents recommend traveling without a debit card because it has direct access to your bank account. Having a trusted power of attorney is far less risky than having the wrong person in a foreign country end up with direct access to all of your cash.
While you’re talking to your attorney, it’s perfectly reasonable to make sure your medical power of attorney is up to date, so that someone can make healthcare decisions for you if you’re incapacitated. And while you’re at it, a living will tells healthcare facilities what your treatment wishes are in the event you are not able to make them for yourself, and relieves loved one from the burden of guessing if you’d have wanted certain life-saving treatments. Lastly, your will states what happens to your assets and life savings, and who should have responsibility for minor children. Don’t rely on verbal instructions that won’t hold up in court, and don’t leave these things to chance.
The challenge you’ll run into is ensuring that a facility in a foreign country will accept your documents created with US and state laws in mind. You should plan to travel with copies of them, but you should also ask the facility you’re considering what their policy is in the event that you are incapacitated and can’t make decisions for yourself. If the person making decisions for you is thousands of miles away, you should have a conversation with them in advance about whether that’s something they are prepared for. You should also ensure that’s acceptable to the facility you’ll use.
Bottom line: is it right for you?
Medical tourism makes the most sense when the procedure is planned and non-urgent, the financial gap between US costs and abroad is large, you have the financial exposure to make the savings matter, you're willing to do the research to find an accredited facility, and you can honestly manage the logistical and emotional reality of receiving care far from home.
It makes the least sense when you're in genuine financial hardship (US safety nets may serve you better), when your condition is urgent or emergent, when you're mid-stream in an existing treatment relationship, or when the procedure is low enough cost that the travel overhead eats the savings.
The American medical establishment doesn't condemn medical tourism. Their concerns about records transfer, infection risk at unaccredited facilities, continuity of care are legitimate and worth taking seriously. But the decision falls to you, and you must advocate for your own physical and financial health.
The conversation to have with yourself is whether you're the person this option was built for. For the right person, in the right financial situation, pursuing the right procedure at a credentialed facility works.
Scot Whiskeyman, CFP® is co-founder of Providers & Families Wealth Management. Together with his wife and business partner Lindsey, they help clients nationwide navigate complex financial decisions — including the ones nobody else wants to talk about.
If you're working through a situation where healthcare costs are creating real financial strain, we're happy to talk through it.
Disclosures
Providers & Families Wealth Management has made every effort to ensure the accuracy of the information contained in this post, but it is provided “as is” and its accuracy cannot be guaranteed. This content is provided for informational and educational purposes only and should not be relied upon as medical, legal, tax, or financial advice. Medical treatment decisions involve complex individual factors and should be made in consultation with qualified healthcare providers. All cost figures are approximate and subject to change; individual quotes from specific facilities may vary significantly from ranges cited. Exchange rate conversions are approximate. External links are provided as a convenience; Providers & Families Wealth Management has no affiliation with linked websites and makes no representations regarding the accuracy, completeness, or security of their content.References
American Medical Association. (2018). AMA adopts ethical guidance on medical tourism. AMA Press Center. https://www.ama-assn.org/press-center/ama-press-releases/ama-adopts-ethical-guidance-medical-tourismAmerican Medical Association. (2018). Medical tourism [Ethics opinion]. AMA Code of Medical Ethics. https://code-medical-ethics.ama-assn.org/ethics-opinions/medical-tourismAmerican College of Surgeons. (2009). Medical and surgical tourism [Position statement]. https://www.facs.org/about-acs/statements/medical-and-surgical-tourism/Bookimed. (2026, February). Hip replacement costs around the world: affordable medical tourism options [Based on internal database analysis of 12,450 patient requests across 9 accredited clinics]. https://us-uk.bookimed.com/article/hip-replacement-costs-around-the-world/Bookimed. (2025). Cheapest countries for hip replacement surgery in 2026. https://curemeabroad.com/blogs/hip-replacement-cost-worldwide-affordable-countries-2026Centers for Disease Control and Prevention. (2025, April 23). Medical tourism. In E. S. Halsey, K. M. Angelo, E. D. Barnett, et al. (Eds.), CDC Yellow Book, 2026 edition: Health Information for International Travel. https://www.ncbi.nlm.nih.gov/books/NBK620895/Centers for Disease Control and Prevention. (2024, January). Deaths of U.S. citizens undergoing cosmetic surgery — Dominican Republic, 2009–2022. Morbidity and Mortality Weekly Report, 73(3). https://www.cdc.gov/mmwr/volumes/73/wr/mm7303a3.htmCenters for Disease Control and Prevention. (2024). Medical tourism. Travelers' Health. https://wwwnc.cdc.gov/travel/page/medical-tourismDentaVacation. (2026, April 13). Cheap dental implants abroad: affordable, safe, high quality [Medically reviewed by Dr. Jonathan Biderman, DDS]. https://www.dentavacation.com/low-cost-dental-implants-abroad/Dentaly.org. (2025). Cheap dental implants abroad — dental tourism. https://www.dentaly.org/us/dental-tourism-usa/Fertility Clinics Abroad. (2026, January 5). Cheapest IVF in Europe — updated 2026. https://www.fertilityclinicsabroad.com/ivf-costs/surprising-cost-ivf-europe/Fertility Road. (2026, February 3). Cheapest IVF in the world: IVF costs by country in 2026. https://fertilityroad.com/treatment-options-abroad/ivf-cost-explained/Frontiers in Psychology. (2022). The importance of social support, optimism and resilience on the quality of life of cancer patients. Frontiers in Psychology, 12. https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2022.833176/fullGold, J. (2024, October). Infection continues to be biggest risk from medical tourism [Presentation, ID Week 2024]. Managed Healthcare Executive. https://www.managedhealthcareexecutive.com/view/infection-continues-to-be-biggest-risk-from-medical-tourism-id-week-2024Health Affairs. (2024). US nonprofit hospitals have widely varying criteria to decide who qualifies for free and discounted charity care. Health Affairs Journal. https://www.healthaffairs.org/doi/10.1377/hlthaff.2023.01615KFF. (2024). The burden of medical debt in the United States. Peterson-KFF Health System Tracker. https://www.healthsystemtracker.org/brief/the-burden-of-medical-debt-in-the-united-states/KFF / AARP. (2023). 5 things you should know about dental health and Medicare. AARP. https://www.aarp.org/medicare/dental-coverage/Lighter Dream. (2026). Bariatric surgery cost Mexico 2026: complete pricing from $3,898. https://lighterdream.com/bariatric-surgery-cost-mexico-guide/McAuliffe, P. B., Muss, T. E. L., Desai, A. A., Talwar, A. A., Broach, R. B., & Fischer, J. P. (2023). Complications of aesthetic surgical tourism treated in the USA: A systematic review. Aesthetic Plastic Surgery, 47, 455–464. https://doi.org/10.1007/s00266-022-03041-zMedical Tourism Co. (2025). Gastric bypass surgery cost abroad: Mexico, India, USA, Australia. https://www.medicaltourismco.com/gastric-bypass-surgery-cost/Medicare.gov. (2024). Medicare coverage outside the United States [Fact sheet]. https://www.medicare.gov/publications/11037-medicare-coverage-outside-the-united-states.pdfMedicare.org. (2025, February 19). Does Medicare cover international travel?https://www.medicare.org/articles/will-medicare-cover-my-healthcare-needs-while-traveling-abroad/Mednfly. (2026, February 8). Invisalign cost comparison: prices in USA, UK, Germany, Thailand and Turkey. https://mednfly.com/blog/mednfly-academy/invisalign-cost-comparisonMedical Tourism Association. (2024). Medical tourism patient survey 2024. International Healthcare Research Center. https://www.healthcareresearchcenter.org/patient-surveyMedical Tourism Magazine. (n.d.). Orthodontics abroad: a guide to braces and aligners in dental tourism destinations. https://www.magazine.medicaltourism.com/article/orthodontics-abroad-a-guide-to-braces-and-aligners-in-dental-tourism-destinationsNational Cancer Institute / American Cancer Society. (2025). When to start cancer treatment. https://www.cancer.org/cancer/managing-cancer/making-treatment-decisions/when-treatment-should-start.htmlNPR / Goats and Soda. (2024, February 22). Risks of medical tourism depicted in report on deadly fungal meningitis. https://www.npr.org/sections/goatsandsoda/2024/02/22/1232959262/medical-tourism-cosmetic-surgery-fungal-meningitis-clinics-mexicoOrthoInfo / American Academy of Orthopaedic Surgeons. (n.d.). What to know about medical tourism. https://www.orthoinfo.org/en/treatment/what-to-know-about-medical-tourism/Paubox. (2025, June 4). HIPAA fundamentals and jurisdictional impact on medical tourism. https://www.paubox.com/blog/hipaa-fundamentals-and-jurisdictional-impact-on-medical-tourismPatients Beyond Borders. (2025). Medical tourism statistics and facts (2026). Media Market US. https://media.market.us/medical-tourism-statistics/Saving Advice. (2025, October 19). Why dental coverage lapses are breaking senior budgets. https://www.savingadvice.com/articles/2025/10/19/10168846_why-dental-coverage-lapses-are-breaking-senior-budgets.htmlSchaeffer, J. (2023). Medical tourism can get you healthcare bargains abroad. Kiplinger. https://www.kiplinger.com/personal-finance/insurance/medical-tourism-can-get-you-healthcare-bargainsSnyder, J., Dharamsi, S., & Crooks, V. A. (2011). Fly-by medical care: Conceptualizing the global and local social responsibilities of medical tourists and physician travelers. Philosophy, Ethics, and Humanities in Medicine, 6(1), 1–14.Sylk Health. (2026). Medical tourism insurance: what coverage you need (2026). https://sylkhealth.com/blog/articles/medical-tourism-insuranceTurkey Luxury Clinics. (2026). Dental implants abroad packages: prices, deals and savings 2026. https://turkeyluxuryclinics.com/en/blog/dental-implants-abroad-packagesTurkey Luxury Clinics. (2026). Cheapest place to get All-on-4 dental implants 2026 options. https://turkeyluxuryclinics.com/en/blog/cheapest-place-to-get-all-on-4-dental-implantsUniversal Medical Travel. (2026, January 2). Cheapest countries for hip replacement surgery in 2026. https://universalmedicaltravel.com/cheapest-countries-for-hip-replacement-surgery-in-the-world/Universal Medical Travel. (2026, January 2). Cheapest places to get dental implants in 2026. https://universalmedicaltravel.com/cheapest-countries-for-dental-implants-in-the-world/U.S. Department of State. (2026). U.S. Passports. Travel.state.gov. https://travel.state.gov/content/travel/en/passports.htmlWorld Medical Tour. (2026, January 4). Medical tourism insurance 2026: complication coverage guide. https://wmedtour.com/medical-tourism-insurance-complication-coverage/World Population Review. (2026). Hip replacement cost by country 2026. https://worldpopulationreview.com/country-rankings/hip-replacement-cost-by-countryOvu.com. (2026, January 31). Fertility tourism 2025: IVF abroad costs, laws and destinations. https://ovu.com/fertility-insights/fertility-tourism-2025-ivf-abroad-costs-laws-destinationsOvu.com. (2025, November 17). IVF costs in Eastern Europe 2026: full guide. https://ovu.com/fertility-insights/fertility-treatment-costs-in-eastern-europe-2026-guide